Advanced Surgical & Endocrine Oncology Care by Dr. Lovedeep Singh Chauhan
Parathyroid cancer is one of the rarest endocrine malignancies, yet when it occurs, it can lead to serious and life-threatening metabolic complications. Unlike many cancers that primarily cause problems due to tumor growth alone, parathyroid carcinoma significantly affects the entire body through uncontrolled secretion of parathyroid hormone (PTH), leading to severe hypercalcemia (high blood calcium levels).
Effective treatment requires not only oncologic expertise but also a deep understanding of endocrine physiology and complex neck anatomy. Dr. Lovedeep Singh Chauhan, Consultant Surgical Oncologist at Max Super Speciality Hospital, Mohali, provides comprehensive and evidence-based management for patients diagnosed with parathyroid cancer and other endocrine malignancies.
This page offers detailed information about parathyroid cancer—its causes, symptoms, diagnosis, treatment, prognosis, and surgical options—while outlining the advanced care approach available under Dr. Chauhan’s expertise.
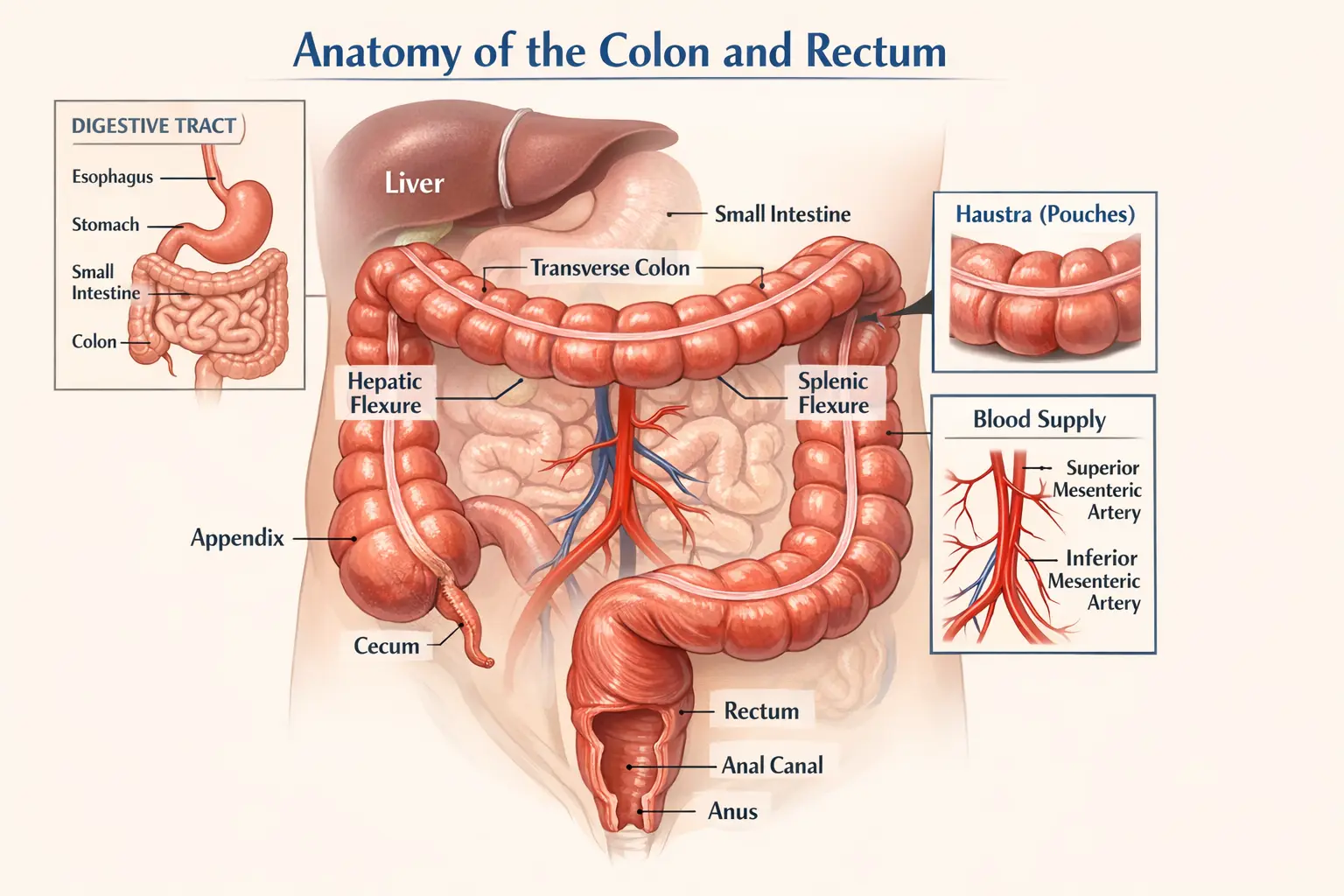
Understanding the Parathyroid Glands
The human body typically has four small parathyroid glands located behind the thyroid gland in the neck. These glands are responsible for regulating calcium levels in the bloodstream through the production of parathyroid hormone (PTH).
- Bone strength
- Muscle contraction
- Nerve conduction
- Heart rhythm regulation
- Blood clotting
When parathyroid glands function normally, they maintain precise calcium balance. However, in parathyroid cancer, the malignant gland produces excessive PTH, leading to dangerously elevated calcium levels.
What Is Parathyroid Cancer?
Parathyroid cancer, also known as parathyroid carcinoma, is a rare malignant tumor arising from one of the parathyroid glands. It accounts for less than 1% of cases of primary hyperparathyroidism.
- Locally invasive
- Associated with extremely high calcium levels
- Prone to recurrence
- Potentially life-threatening if untreated
The condition requires early recognition and definitive surgical management for optimal outcomes.
Causes and Risk Factors
The exact cause of parathyroid cancer remains unclear, but certain genetic and clinical factors are associated with increased risk.
Genetic Associations
Some patients may have inherited conditions such as:
- Hyperparathyroidism-Jaw Tumor (HPT-JT) syndrome
- CDC73 gene mutation
These genetic abnormalities can predispose individuals to parathyroid carcinoma.
Sporadic Cases
Most cases occur without a clear hereditary cause.
Long-standing untreated hyperparathyroidism may also contribute to increased risk.
Symptoms of Parathyroid Cancer
The majority of symptoms arise from severe hypercalcemia rather than the tumor mass itself.
Early Symptoms
Patients may initially experience:
- Persistent fatigue and weakness
- Increased thirst and frequent urination
- Loss of appetite
- Nausea and constipation
- Mood disturbances
Advanced Symptoms
As calcium levels rise further, symptoms may include:
- Recurrent kidney stones
- Bone pain and fractures
- Abdominal pain
- Cognitive impairment or confusion
- Cardiac rhythm abnormalities
- Palpable neck swelling
How Parathyroid Cancer Is Diagnosed
Accurate diagnosis is critical because incomplete surgery significantly increases the risk of recurrence.
Biochemical Evaluation
The first step usually involves blood tests showing:
- Markedly elevated serum calcium
- Extremely high PTH levels
- Abnormal kidney function tests
Calcium levels in parathyroid cancer are often higher than those seen in benign adenomas.
Imaging Studies
Imaging helps localize the tumor and assess local invasion. Common investigations include:
- Neck ultrasound
- Sestamibi scan
- CT scan or MRI of the neck and chest
- PET-CT in selected or recurrent cases
Histopathological Confirmation
Definitive diagnosis is usually established after surgical removal of the tumor. Pathologists look for features such as:
- Capsular invasion
- Vascular invasion
- Local tissue infiltration
Fine needle aspiration (FNAC) is generally avoided due to the risk of tumor seeding.
Staging and Disease Extent
Because parathyroid cancer is rare, staging systems are less standardized compared to other cancers. However, evaluation typically focuses on:
Local invasion into thyroid, trachea, esophagus, or soft tissues
Lymph node involvement
Distant metastasis (lungs, liver, bones)
Early-stage disease confined to the gland has the best prognosis when completely removed.
Treatment of Parathyroid Cancer
Surgery remains the cornerstone of treatment and offers the best chance of cure.
Surgery – The Cornerstone of Cure
Surgery is the only potentially curative treatment for parathyroid carcinoma.
The recommended approach is en bloc resection, meaning removal of:
- The affected parathyroid gland
- Adjacent thyroid lobe if involved
- Surrounding soft tissues if invaded
- Involved lymph nodes (if necessary)
Complete removal during the first surgery significantly improves long-term survival, while incomplete excision increases recurrence rates dramatically.
Management of Severe Hypercalcemia
Before surgery, patients often require stabilization of calcium levels.
Treatment may include:
- Intravenous fluids
- Bisphosphonates
- Calcitonin
- Dialysis in critical cases
Post-operatively, calcium levels must be closely monitored because sudden drops may occur (hungry bone syndrome).
Role of Radiotherapy and Chemotherapy
Parathyroid cancer is generally resistant to conventional chemotherapy.
Incomplete tumor resection
Local recurrence
Positive surgical margins
Radiotherapy may be considered in selected cases. Targeted therapies are currently under research and are not yet part of standard treatment.
Recurrence and Long-Term Monitoring
Parathyroid carcinoma has a relatively high risk of recurrence, sometimes years after initial surgery.
Regular serum calcium monitoring
Periodic PTH level checks
Imaging when indicated
Early detection of recurrence allows timely intervention.
Surgical Expertise in Endocrine Oncology
The anatomy of the neck is complex and contains critical structures requiring high surgical precision.
Precision & Surgical Expertise
- Recurrent laryngeal nerve (voice nerve)
- Major blood vessels
- Trachea and esophagus
- Complete tumor removal
- Preservation of nerve function
- Prevention of complications
- Reduced recurrence risk
Dr. Lovedeep Singh Chauhan has extensive experience in endocrine malignancies including thyroid and parathyroid cancers, with training from leading oncology institutes ensuring evidence-based care.
Why Choose Dr. Lovedeep Singh Chauhan?
- Multidisciplinary treatment approach
- Comprehensive diagnostic evaluation
- Advanced imaging facilities
- Modern operating infrastructure
- Intensive perioperative monitoring
- Structured long-term follow-up
His approach focuses on accurate diagnosis, individualized surgical planning, complete oncologic resection, postoperative metabolic stabilization, and lifelong surveillance.
What to Expect During Treatment
A structured and carefully monitored approach ensures safe and effective treatment outcomes.
Initial Consultation
A detailed review of symptoms, previous reports, and biochemical values is performed. Imaging studies are evaluated to determine disease extent.
Preoperative Optimization
If calcium levels are significantly elevated, stabilization is done before surgery to reduce perioperative risks.
Surgical Procedure
Surgery is performed under general anesthesia. En bloc resection may be done depending on disease extent to ensure complete removal.
Postoperative Care
- Calcium level monitoring
- Voice assessment
- Wound healing
- Metabolic stability
Most patients gradually return to normal activities under medical guidance.
Prognosis and Survival
Prognosis depends on multiple clinical and surgical factors that influence long-term outcomes.
Completeness of initial surgery
Tumor invasion
Presence of metastasis
Biochemical control of calcium
Patients who undergo complete en bloc resection during the first surgery generally have significantly better long-term outcomes.
When Should You Seek Expert Evaluation?
Early consultation with a specialist can significantly improve outcomes and reduce complications.
Very high calcium levels
Persistent hyperparathyroidism after surgery
Recurrent kidney stones with high PTH
Suspected parathyroid tumor on imaging
Neck swelling with biochemical abnormalities
Early referral improves surgical success and reduces complications.