Understanding Invasive Ductal Carcinoma
Invasive Ductal Carcinoma (IDC) is the most common type of breast cancer, accounting for approximately 70–80% of all invasive breast malignancies. It begins in the milk ducts of the breast and invades surrounding breast tissue. Unlike Ductal Carcinoma In Situ (DCIS), which remains confined within the ducts, IDC has crossed the duct wall and gained the ability to infiltrate nearby structures and potentially spread to lymph nodes or distant organs.
A diagnosis of IDC can feel overwhelming. However, advances in surgical oncology, molecular testing, targeted therapy, and personalized treatment planning have significantly improved survival rates and quality of life. With early detection and evidence-based management, many patients achieve long-term remission and cure.
Dr. Lovedeep Singh Chauhan at Max Super Speciality Hospital, treatment for Invasive Ductal Carcinoma is delivered through a multidisciplinary, patient-centered approach under the care of Dr. Lovedeep Singh Chauhan, Consultant Surgical Oncologist specializing in breast cancer and advanced oncologic surgery.
Breast Anatomy and How IDC Develops
To understand IDC, it is important to know how the breast is structured. The breast consists of lobules (milk-producing glands), ducts (which carry milk to the nipple), connective tissue, fat, lymphatic channels, and blood vessels. IDC begins when abnormal cells develop within the lining of the ducts.
Over time, these abnormal cells multiply uncontrollably and break through the duct wall into surrounding tissue. Once invasive, the cancer can:
- Form a palpable lump
- Spread to axillary (underarm) lymph nodes
- Enter blood vessels and metastasize to distant organs such as bone, liver, lung, or brain
The transition from non-invasive to invasive disease marks a critical stage where timely treatment becomes essential.

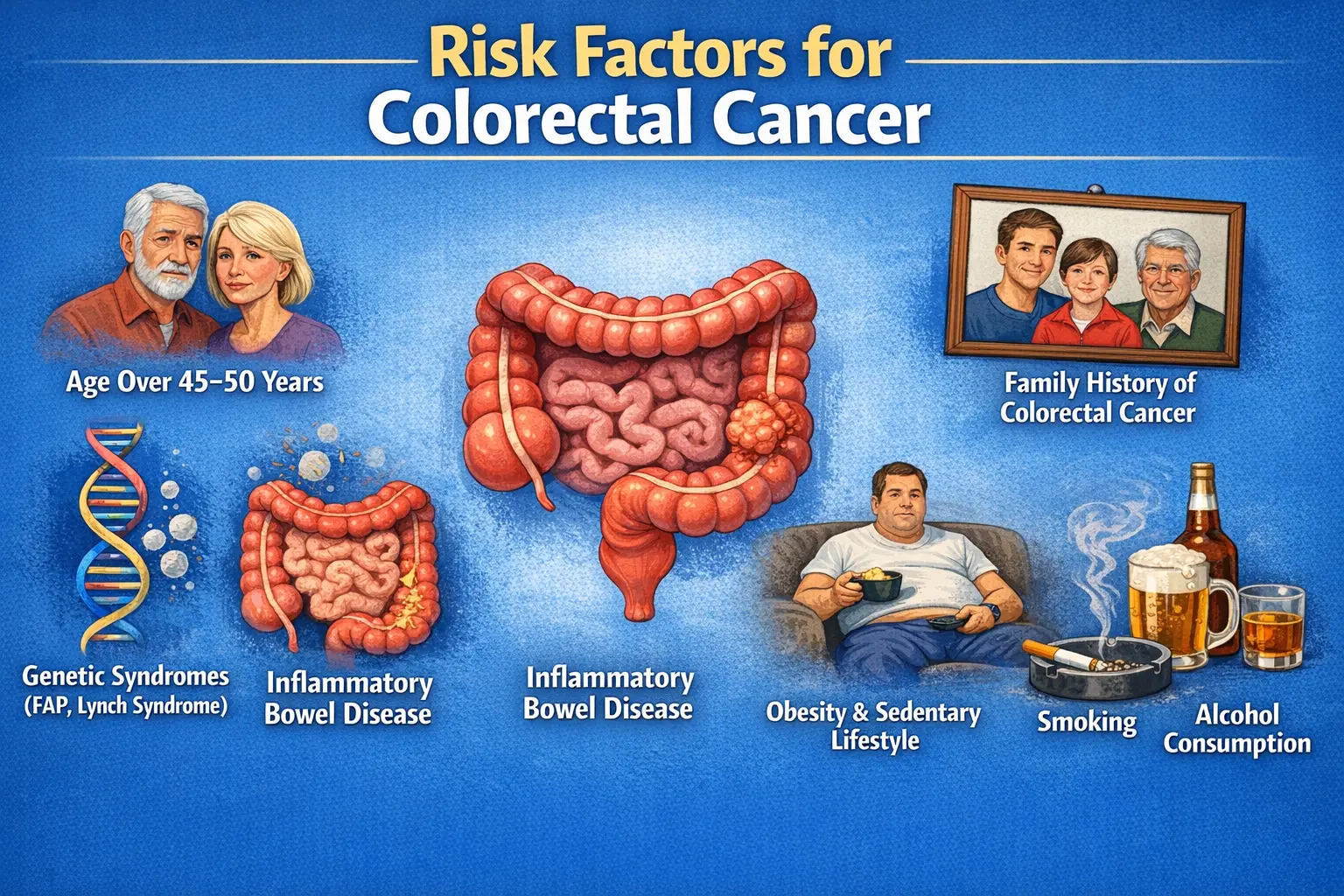
Risk Factors for Invasive Ductal Carcinoma
While IDC can occur without identifiable risk factors, several conditions increase the likelihood of developing breast cancer:
Age is one of the strongest risk factors. The risk increases significantly after 40 years. Family history of breast or ovarian cancer also plays a major role, especially when associated with BRCA1 or BRCA2 gene mutations. Hormonal factors such as early menarche, late menopause, and prolonged hormone replacement therapy increase cumulative estrogen exposure. Obesity, lack of physical activity, alcohol consumption, and previous radiation exposure to the chest are also recognized contributors.
It is important to understand that having risk factors does not mean a person will definitely develop IDC. Likewise, many patients diagnosed with IDC may not have obvious risk factors.
Symptoms of Invasive Ductal Carcinoma
IDC may present in various ways. In early stages, it may not cause noticeable symptoms and may only be detected on routine screening mammography. As the disease progresses, patients may notice:
A painless lump in the breast is the most common presentation. Changes in breast size or shape, skin dimpling, puckering, redness, nipple retraction, or bloody nipple discharge may also occur. Some patients may feel swelling or lumps in the underarm region due to lymph node involvement.
Any persistent breast change should be evaluated promptly by a specialist.
Diagnostic Evaluation and Staging
Accurate diagnosis and staging are the foundation of effective breast cancer treatment.
The evaluation begins with a clinical breast examination followed by imaging. Mammography remains the gold standard screening tool. Ultrasound helps characterize lumps, especially in dense breasts. MRI of the breast may be recommended in selected cases to assess multifocal or bilateral disease.
Definitive diagnosis requires a core needle biopsy. The tissue sample undergoes histopathological examination to confirm IDC. Importantly, the biopsy also assesses hormone receptor status (ER and PR), HER2 expression, and Ki-67 proliferation index. These markers determine tumor biology and guide treatment decisions.
Staging investigations may include CT scans, PET-CT, or bone scans depending on tumor stage and symptoms. Breast cancer staging follows the TNM system—evaluating tumor size, lymph node involvement, and distant metastasis.
Molecular Subtypes of IDC
IDC is not a single disease but a biologically diverse condition. Molecular classification plays a vital role in treatment planning.
Hormone receptor-positive cancers express estrogen or progesterone receptors and often respond well to hormone therapy. HER2-positive cancers overexpress the HER2 protein and benefit from targeted therapy such as trastuzumab. Triple-negative breast cancer lacks ER, PR, and HER2 expression and may require chemotherapy and immunotherapy strategies.
Understanding tumor biology allows for precision medicine—offering therapies tailored to the individual patient.

Treatment of Invasive Ductal Carcinoma
Treatment for IDC is individualized and typically involves a combination of surgery, systemic therapy, and radiation therapy. The sequence and type of treatment depend on stage, tumor biology, and patient-specific factors.
At Max Super Speciality Hospital, patients benefit from a multidisciplinary tumor board approach where surgical oncologists, medical oncologists, radiation oncologists, radiologists, and pathologists collaborate to formulate optimal treatment plans.
Surgical Management of IDC
Surgery remains the cornerstone of curative treatment for localized Invasive Ductal Carcinoma.
Breast-Conserving Surgery (Lumpectomy)
For appropriately selected patients, breast-conserving surgery allows removal of the tumor with a margin of healthy tissue while preserving most of the breast. This is typically followed by radiation therapy. Numerous studies show equivalent survival outcomes between lumpectomy with radiation and mastectomy in early-stage disease.
Modified Radical Mastectomy
In cases where the tumor is large, multifocal, or unsuitable for conservation, removal of the entire breast may be required. Axillary lymph node evaluation is performed simultaneously.
Sentinel Lymph Node Biopsy
Sentinel node biopsy identifies the first lymph nodes that drain the breast. If these nodes are cancer-free, extensive node removal may be avoided, reducing complications such as lymphedema.
Breast Reconstruction
Reconstruction can be performed immediately or delayed. Options include implant-based reconstruction or autologous tissue reconstruction. Modern oncoplastic techniques aim to maintain cosmetic outcomes without compromising cancer control.
Dr. Lovedeep Singh Chauhan emphasizes oncologic safety while preserving body image and quality of life wherever possible.
Chemotherapy in IDC
Chemotherapy may be administered before surgery (neoadjuvant chemotherapy) to shrink tumors and enable breast conservation. It may also be given after surgery (adjuvant chemotherapy) to eliminate microscopic disease and reduce recurrence risk.
The decision depends on tumor size, lymph node status, molecular subtype, and genomic testing results.
Neoadjuvant therapy also provides valuable information about tumor response, particularly in HER2-positive and triple-negative cancers.
Hormone Therapy
For hormone receptor-positive IDC, endocrine therapy plays a critical role. Medications such as tamoxifen or aromatase inhibitors reduce estrogen-driven tumor growth. Hormone therapy is typically continued for 5–10 years depending on risk assessment.
This long-term therapy significantly reduces recurrence risk and improves survival outcomes.
Targeted Therapy and Immunotherapy
HER2-positive cancers benefit from HER2-targeted agents such as trastuzumab, often combined with chemotherapy. These targeted treatments have dramatically improved outcomes in HER2-driven disease.
Triple-negative breast cancers may benefit from immunotherapy in selected cases, particularly in advanced stages.
Precision oncology continues to evolve, offering newer targeted agents and antibody-drug conjugates for specific subtypes.
Radiation Therapy
Radiation therapy is typically recommended after breast-conserving surgery. It may also be indicated after mastectomy in patients with large tumors or multiple positive lymph nodes.
Radiation reduces local recurrence and improves long-term disease control.
Prognosis and Survival
The prognosis of Invasive Ductal Carcinoma depends largely on stage at diagnosis and tumor biology. Early-stage IDC has excellent survival rates with appropriate treatment. Even in advanced stages, modern systemic therapies can provide meaningful disease control and prolonged survival.
Regular follow-up care is essential for early detection of recurrence and management of long-term therapy effects.
Survivorship and Long-Term Care
Breast cancer treatment does not end with surgery or chemotherapy. Survivorship care includes regular clinical examinations, imaging surveillance, management of therapy side effects, bone health monitoring, and psychological support.
Lifestyle modification—including regular exercise, balanced nutrition, weight management, and avoidance of tobacco—plays a significant role in long-term health.
Dr. Lovedeep Singh Chauhan ensures structured follow-up protocols tailored to each patient’s risk profile.
Why Choose Dr. Lovedeep Singh Chauhan for IDC Treatment?
Invasive Ductal Carcinoma requires expertise, precision, and compassionate care. Dr. Lovedeep Singh Chauhan is a Consultant Surgical Oncologist with advanced training in breast cancer surgery and multidisciplinary oncologic management.
Practicing at Max Super Speciality Hospital, he offers:
Evidence-based treatment planning
Advanced breast-conserving and oncoplastic surgery
Sentinel lymph node mapping
Coordinated care with medical and radiation oncology teams
Personalized counseling and long-term follow-up
Patients receive comprehensive care under one roof with access to modern diagnostics, advanced operating infrastructure, and supportive oncology services.
Book a Consultation
If you or a loved one has been diagnosed with Invasive Ductal Carcinoma, early specialist consultation is critical. Timely evaluation, accurate staging, and personalized treatment planning significantly improve outcomes.
To schedule an appointment with Dr. Lovedeep Singh Chauhan, visit Max Super Speciality Hospital and begin your journey toward comprehensive, evidence-based breast cancer care.